Determinants of Low Birth Weight Sex of Babies
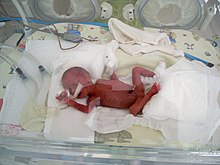
Low nascence weight (LBW) is divers by the World Wellness System as a birth weight of an baby of two,499 thousand (5 lb viii.1 oz) or less, regardless of gestational age.[one] Infants built-in with LBW have added wellness risks which crave shut direction, often in a neonatal intensive care unit (NICU). They are as well at increased risk for long-term health atmospheric condition which require follow-upwardly over time.
Nomenclature [edit]
Nativity weight may be classified as:[2]
- High birth weight (macrosomia): greater than 4,200 m (9 lb 4 oz)
- Normal weight (term delivery): 2,500–4,200 thou (5 lb 8 oz – nine lb iv oz)
- Depression birth weight: less than 2,500 g (5 lb 8 oz)
- Very low birth weight: less than one,500 g (iii lb five oz)
- Extremely low nativity weight: less than one,000 g (ii lb 3 oz)
Causes [edit]
LBW is either caused by preterm nascence (that is, a low gestational historic period at nativity, unremarkably defined equally younger than 37 weeks of gestation) or the infant existence pocket-size for gestational age (that is, a deadening prenatal growth rate), or a combination of both.[ commendation needed ]
In general, risk factors in the mother that may contribute to depression birth weight include immature ages, multiple pregnancies, previous LBW infants, poor diet, heart disease or hypertension, untreated celiac disease, substance use disorder, excessive booze use, and insufficient prenatal care. It can as well be caused past prelabor rupture of membranes.[3] Environmental adventure factors include smoking, lead exposure, and other types of air pollutions.[iv] [5] [vi]
Preterm nascence [edit]
The machinery of preterm birth is heterogeneous and poorly understood. It may be tied to one or more of the post-obit processes: premature fetal endocrine activation, intrauterine inflammation, over-distension of the uterus, and endometrial bleeding. A prominent take chances factor for preterm birth is prior history of preterm commitment. However, there is no reliable protocol for screening and prevention of preterm nascency.[7]
Small for gestational age [edit]
Infants built-in small-scale for gestational age may exist constitutionally small, with no associated pathologic procedure. Others have intrauterine growth brake (IUGR) due to any of diverse pathologic processes. Babies with chromosomal abnormalities or other built anomalies may manifest IUGR every bit part of their syndrome. Problems with the placenta can prevent it from providing acceptable oxygen and nutrients to the fetus, resulting in growth brake. Infections during pregnancy that affect the fetus, such as rubella, cytomegalovirus, toxoplasmosis, and syphilis, may also impact the baby's weight.[ commendation needed ]
Ecology factors [edit]
Maternal tobacco smoking doubles take chances of LBW for the infant.[viii] More than recently, passive maternal smoking has been examined for possible effects on nativity weight, and has been shown to increase risk of LBW by 16%.[9]
Air pollutants [edit]
The combustion products of solid fuel in developing countries can cause many adverse health issues in people. Because a majority of pregnant women in developing countries, where rate of LBW is high, are heavily exposed to indoor air pollution, increased relative risk translates into substantial population attributable risk of 21% of LBW.[x]
Particulate matter, a component of ambient air pollution, is associated with increased risk of low nativity weight.[11] [12] Considering particulate matter is composed of extremely small particles, even nonvisible levels can be inhaled and present harm to the fetus.[xiii] Particulate thing exposure tin can cause inflammation, oxidative stress, endocrine disruption, and impaired oxygen transport access to the placenta, all of which are mechanisms for heightening the risk of low nascency weight.[xiv] To reduce exposure to particulate matter, pregnant women can monitor the EPA's Air Quality Index and take personal precautionary measures such equally reducing outdoor activity on low quality days, avoiding loftier-traffic roads/intersections, and/or wearing personal protective equipment (i.e., facial mask of industrial design). Indoor exposure to particulate affair tin also be reduced through adequate ventilation, every bit well as use of clean heating and cooking methods.[xv] [16]
A correlation betwixt maternal exposure to carbon monoxide (CO) and depression nascency weight has been reported that the effect on birth weight of increased ambience CO was as large as the consequence of the female parent smoking a pack of cigarettes per day during pregnancy.[17] It has been revealed that adverse reproductive effects (e.one thousand., risk for LBW) were correlated with maternal exposure to CO emissions in Eastern Europe and Northward America.[xviii] Mercury is a known toxic heavy metal that can damage fetal growth and health, and there has been evidence showing that exposure to mercury (via consumption of large oily fish) during pregnancy may exist related to higher risks of LBW in the offspring.[19]
Other exposures [edit]
Elevated blood lead levels in pregnant women, fifty-fifty those well below the US Centers for Illness Control and Prevention's 10 ug/dL "level of business", tin can crusade miscarriage, premature birth, and LBW in the offspring.[20] Exposure of significant women to airplane dissonance was found to be associated with low birth weight via adverse effects on fetal growth.[21] Prevalence of low birth weight in Nippon is associated with radiation doses from the Fukushima accidents of March 2011.[22]
Periodontal health [edit]
Low birth weight, preterm birth and preeclampsia have been associated with maternal periodontal illness, though the strength of the observed associations is inconsistent and varies according to the population studied, the ways of periodontal assessment and the periodontal affliction classification employed.[23] The risk of low birth weight can be reduced with treatment of the periodontal disease. This therapy is prophylactic during pregnancy and reduces the inflammatory burden, thus decreasing run a risk for preterm nascence and depression birth weight.[24]
Management [edit]
Temperature regulation [edit]

Skin-to-skin contact with the mother tin help with thermoregulation.

Low nativity weight babies oftentimes spend time in a temperature-controlled incubator due to their disability to maintain core body temperature.
LBW newborns are at increased risk of hypothermia due to decreased brown fatty stores. Plastic wraps, heated pads, and skin-to-skin contact decrease risk of hypothermia immediately after delivery. One or more of these interventions may be employed, though combinations incur risk of hyperthermia.[25] Warmed incubators in the NICU help in thermoregulation for LBW infants.[ citation needed ]
Fluid and electrolyte balance [edit]
Frequent clinical monitoring of volume status and checking of serum electrolytes (up to 3 times daily) is appropriate to prevent dehydration, fluid overload, and electrolyte imbalance.[26] VLBW newborns take an increased body surface to weight ratio, increasing adventure for insensible fluid losses and dehydration.[27] Humidified incubators and skin emollients can lessen insensible fluid loss in VLBW newborns.[26] However, fluid overloading is not benign; it is associated with increased risk of congestive heart failure, necrotizing enterocolitis, and mortality. A degree of fluid restriction mitigates these risks.[26]
VLBW newborns are at risk for electrolyte imbalances due to the relative immaturity of the nephrons in their kidneys. The kidneys are not equipped to handle large sodium loads. Therefore, if normal saline is given, the sodium level may become elevated, which may prompt the clinician to give more than fluids. Sodium restriction has been shown to prevent fluid overload.[26] Potassium must also be monitored carefully, as immature aldosterone sensitivity and sodium-potassium pumping increases hazard for hyperkalemia and cardiac arrhythmias.[26]
VLBW newborns are frequently found to have a persistently patent ductus arteriosus (PDA). If present, information technology is important to evaluate whether the PDA is causing increased circulatory book, thus posing risk for heart failure. Signs of clinically meaning PDA include widened pulse pressure and bounding pulses. In newborns with significant PDA, fluid brake may avoid the need for surgical or medical therapy to shut it.[26]
Approach to diet [edit]
As their gastrointestinal systems are typically unready for enteral feeds at the time of nascence, VLBW infants require initial parenteral infusion of fluids, macronutrients, vitamins, and micronutrients.[27]
Free energy needs [edit]
Decreased action compared to normal weight newborns may decrease energy requirements, while comorbidities such every bit bronchopulmonary dysplasia may increment them. Daily weight gain can reveal whether a VLBW newborn is receiving adequate calories. Growth of 21 grand/kg/day, mirroring in utero growth, is a target for VLBW and ELBW neonates.[27]
Enteral sources [edit]
Upon transitioning to enteral nutrition, homo milk is preferable to formula initially in VLBW newborns because it speeds up evolution of the intestinal barrier and thereby reduces risk of necrotizing enterocolitis,[27] with an absolute risk reduction of iv%.[28] Donor human milk and maternal expressed breast milk are both associated with this benefit.[29] One drawback of homo milk is the imprecision in its calorie content. The fat content in human milk varies greatly among women; therefore, the free energy content of human milk cannot exist known as precisely as formula.[27] Each time human milk is transferred betwixt containers, some of the fat content may stick to the container, decreasing the free energy content. Minimizing transfers of human milk between containers decreases the amount of energy loss.[27] Formula is associated with greater linear growth and weight gain than donor breast milk in LBW infants.[29]
Individual food considerations [edit]
VLBW newborns are at increased adventure for hypoglycemia due to decreased energy reserves and large brain mass to body mass ratio. Hypoglycemia may be prevented by intravenous infusion of glucose, amino acids, and lipids.[27] These patients are also at risk of hyperglycemia due to young insulin secretion and sensitivity. However, insulin supplementation is not recommended due to the possible adverse effect of hypoglycemia, which is more dangerous.[27]
VLBW newborns accept increased demand for amino acids to mirror in utero nutrition. Daily protein intake above 3.0 one thousand/kg is associated with improved weight gain for LBW infants.[30] ELBW newborns may require as much as 4 1000/kg/day of protein.[27]
Due to the express solubility of calcium and phosphorus in parenteral infusions, VLBW infants receiving parenteral nutrition will be somewhat deficient of these elements and will require clinical monitoring for osteopenia.[27]
Hematology [edit]
One Cochrane review showed administration of erythropoietin (EPO) decreases subsequently need for blood transfusions, and also is associated with protection against necrotizing enterocolitis and intraventricular hemorrhage. EPO is safe and does not increment run a risk of bloodshed or retinopathy of prematurity.[31]
Prognosis [edit]
Perinatal outcomes [edit]
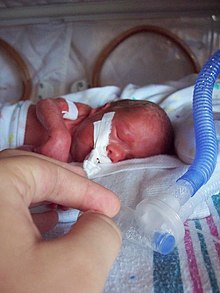
LBW is closely associated with fetal and perinatal bloodshed and morbidity, inhibited growth and cognitive development, and chronic diseases later in life. At the population level, the proportion of babies with a LBW is an indicator of a multifaceted public-health problem that includes long-term maternal malnutrition, ill health, hard work and poor health care in pregnancy. On an individual footing, LBW is an important predictor of newborn health and survival and is associated with college gamble of infant and childhood bloodshed.[32]
Low nascency weight constitutes as sixty to eighty percent of the infant mortality rate in developing countries. Infant mortality due to low nativity weight is usually direct causal, stemming from other medical complications such as preterm birth, PPROM,[33] poor maternal nutritional condition, lack of prenatal care, maternal sickness during pregnancy, and an unhygienic home environment.[34]
Long term outcomes [edit]
Hyponatremia in the newborn period is associated with neurodevelopmental weather such equally spastic cerebral palsy and sensorineural hearing loss. Rapid correction of hyponatremia (faster than 0.four mEq/L/60 minutes) perinatally is as well associated with neurodevelopmental adverse effects.[26] Among VLBW children, run a risk for cerebral impairment is increased with lower nascency weight, male sex, nonwhite ethnicity, and lower parental education level. There is no articulate clan betwixt brain injury in the neonatal catamenia and later cerebral harm.[35] Additionally, low nativity weight has associations with cardiovascular diseases later in life, particularly in cases of large increases in weight during childhood.[36] [37] [38] [39]
Epidemiology [edit]
The World Health Organisation (WHO) estimates the worldwide prevalence of low nativity weight at 15% as of 2014, and varies by region: Sub-Saharan Africa, 13%; South Asia, 28%; Eastern asia and the Pacific, 6%; Latin America and the Caribbean, 9%.[xl] Amass prevalence of LBW in Un-designated To the lowest degree Adult Countries[41] is 13%.[40] The WHO has gear up a goal of reducing worldwide prevalence of LBW by xxx% through public health interventions including improved prenatal care and women's education.[40]
In the U.s.a., the Centers for Affliction Command and Prevention (CDC) reports 313,752 LBW infants in 2018, for a prevalence of eight.28%.[42] This is increased from an estimated half-dozen.ane% prevalence in 2011 past the Agency for Healthcare Research and Quality (AHRQ).[43] The CDC reported prevalence of VLBW at 1.38% in 2018, similar to the 2011 AHRQ estimate.[43]
References [edit]
- ^ P07 - Disorders related to brusque gestation and low birth weight in ICD-10
- ^ "eMedicine - Extremely Low Nativity Weight Infant : Article by KN Siva Subramanian, Medico". Retrieved 2007-11-28 .
- ^ Rizzo, Nicola; Simonazzi, Giuliana; Curti, Alessandra (2015-09-24). "Obstetrical chance factors of ELBW". Italian Journal of Pediatrics. 41 (Suppl 1): A35. doi:x.1186/1824-7288-41-S1-A35. ISSN 1824-7288. PMC4595176.
- ^ "Labor and commitment - Low Birth Weight". Umm.edu. 2008-x-22. Archived from the original on 2011-08-20. Retrieved 2011-01-05 .
- ^ Tersigni, C.; Castellani, R.; de Waure, C.; Fattorossi, A.; De Spirito, M.; Gasbarrini, A.; Scambia, G.; Di Simone, N. (2014). "Celiac disease and reproductive disorders: meta-analysis of epidemiologic associations and potential pathogenic mechanisms". Homo Reproduction Update. xx (4): 582–593. doi:10.1093/humupd/dmu007. ISSN 1355-4786. PMID 24619876.
- ^ Saccone Thousand, Berghella V, Sarno L, Maruotti GM, Cetin I, Greco Fifty, Khashan AS, McCarthy F, Martinelli D, Fortunato F, Martinelli P (Oct ix, 2015). "Celiac affliction and obstetric complications: a systematic review and metaanalysis". Am J Obstet Gynecol. 214 (ii): 225–34. doi:ten.1016/j.ajog.2015.09.080. PMID 26432464.
- ^ Simhan HN, Caritis SN (2007). "Prevention of Preterm Delivery". New England Journal of Medicine. 357 (5): 477–487. doi:10.1056/NEJMra050435. PMID 17671256.
- ^ Knopik, Valerie S. (2009). "Maternal smoking during pregnancy and child outcomes: existent or spurious result?". Developmental Neuropsychology. 34 (1): 1–36. doi:x.1080/87565640802564366. ISSN 1532-6942. PMC3581055. PMID 19142764.
- ^ Salmasi, Giselle; Grady, Rosheen; Jones, Jennifer; McDonald, Sarah D.; Knowledge Synthesis Grouping (2010). "Environmental tobacco smoke exposure and perinatal outcomes: a systematic review and meta-analyses". Acta Obstetricia et Gynecologica Scandinavica. 89 (4): 423–441. doi:10.3109/00016340903505748. ISSN 1600-0412. PMID 20085532. S2CID 9206564.
- ^ Pope, Daniel P.; Mishra, Vinod; Thompson, Lisa; Siddiqui, Amna Rehana; Rehfuess, Eva A.; Weber, Martin; Bruce, Nigel G. (2010). "Risk of depression birth weight and stillbirth associated with indoor air pollution from solid fuel use in developing countries". Epidemiologic Reviews. 32: 70–81. doi:10.1093/epirev/mxq005. ISSN 1478-6729. PMID 20378629.
- ^ EPA, OAR, United states (2014-04-09). "Criteria Air Pollutants". www.epa.gov . Retrieved 2017-03-31 .
- ^ Li, Xiangyu; Huang, Shuqiong; Jiao, Anqi; Yang, Xuhao; Yun, Junfeng; Wang, Yuxin; Xue, Xiaowei; Chu, Yuanyuan; Liu, Feifei; Liu, Yisi; Ren, Meng (Aug 2017). "Clan between ambient fine particulate matter and preterm birth or term depression birth weight: An updated systematic review and meta-analysis". Environmental Pollution (Barking, Essex: 1987). 227: 596–605. doi:ten.1016/j.envpol.2017.03.055. ISSN 1873-6424. PMID 28457735.
- ^ "CDC - Air Quality - Particle Pollution". world wide web.cdc.gov . Retrieved 2017-03-31 .
- ^ Erickson, Anders C.; Arbour, Laura (2014-11-26). "The Shared Pathoetiological Effects of Particulate Air Pollution and the Social Environs on Fetal-Placental Development". Journal of Environmental and Public Health. 2014: 901017. doi:ten.1155/2014/901017. ISSN 1687-9805. PMC4276595. PMID 25574176.
- ^ "Particulate affair". EPA. 2009-05-19. Archived from the original on 2009-06-04.
- ^ US EPA National Centre for Ecology Assessment, Enquiry Triangle Park NC, Environmental Media Assessment Group; Sacks, Jason. "2009 Final Report: Integrated Science Assessment for Particulate Matter". cfpub.epa.gov . Retrieved 2017-03-31 .
{{cite web}}: CS1 maint: multiple names: authors list (link) - ^ Lewtas, Joellen (November 2007). "Air pollution combustion emissions: characterization of causative agents and mechanisms associated with cancer, reproductive, and cardiovascular effects". Mutation Research. 636 (1–3): 95–133. doi:10.1016/j.mrrev.2007.08.003. ISSN 0027-5107. PMID 17951105.
- ^ Townsend CL, Maynard RL (Oct 2002). "Effects on health of prolonged exposure to low concentrations of carbon monoxide". Occup Environ Med. 59 (x): 708–11. doi:10.1136/oem.59.10.708. PMC1740215. PMID 12356933.
- ^ Gochfeld M, Burger J (Aug 2005). "Proficient fish/bad fish: a composite benefit-take chances by dose curve". Neurotoxicology. 26 (iv): 511–20. doi:10.1016/j.neuro.2004.12.010. PMID 15979722.
- ^ Cleveland, Lisa M.; Minter, Monica L.; Cobb, Kathleen A.; Scott, Anthony A.; German, Victor F. (Oct 2008). "Pb hazards for significant women and children: part ane: immigrants and the poor shoulder nigh of the brunt of pb exposure in this country. Role 1 of a ii-part commodity details how exposure happens, whom information technology affects, and the harm it can do". The American Periodical of Nursing. 108 (10): 40–49, quiz 50. doi:10.1097/01.NAJ.0000337736.76730.66. ISSN 1538-7488. PMID 18827541.
- ^ Kawada T (February 2004). "The consequence of noise on the health of children". Journal of Nippon Medical School. 71 (1): 5–10. doi:x.1272/jnms.71.5. PMID 15129589.
- ^ Scherb H, Hayashi Grand (July 2020). "Spatiotemporal association of low birth weight with Cs-137 deposition at the prefecture level in Japan after the Fukushima nuclear power plant accidents: an belittling-ecologic epidemiological written report". Environmental Health. 19 (i): 82. doi:10.1186/s12940-020-00630-due west. PMC7346451. PMID 32646457.
- ^ Sanz, K (Apr 2013). "Periodontitis and adverse pregnancy outcomes: consensus report of the Articulation EFP/AAP Workshop on Periodontitis and Systemic Diseases". J Periodontol. 84 (four suppl): S164–nine. doi:ten.1902/jop.2013.1340016. PMID 23631576.
- ^ Shah, Monali (November 2013). "Upshot of nonsurgical periodontal therapy during gestation period on adverse pregnancy outcome: a systematic review". J Matern Fetal Neonatal Med. 26 (17): 1691–5. doi:10.3109/14767058.2013.799662. PMID 23617740. S2CID 23564952.
- ^ McCall, Emma Yard.; Alderdice, Fiona; Halliday, Henry Fifty.; Vohra, Sunita; Johnston, Linda (12 Feb 2018). "Interventions to prevent hypothermia at birth in preterm and/or low nascency weight infants". The Cochrane Database of Systematic Reviews. 2018 (2): CD004210. doi:10.1002/14651858.CD004210.pub5. ISSN 1469-493X. PMC6491068. PMID 29431872.
- ^ a b c d e f one thousand Evidence-based handbook of neonatology. Oh, William. New Jersey: World Scientific. 2011. pp. 267–290. ISBN978-981-4313-46-9. OCLC 775591575.
{{cite book}}: CS1 maint: others (link) - ^ a b c d eastward f m h i j Bear witness-based handbook of neonatology. Oh, William. New Jersey: World Scientific. 2011. pp. 291–315. ISBN978-981-4313-46-9. OCLC 775591575.
{{cite volume}}: CS1 maint: others (link) - ^ Miller, Jacqueline; Tonkin, Emma; Damarell, Raechel A.; McPhee, Andrew J.; Suganuma, Machiko; Suganuma, Hiroki; Middleton, Philippa F.; Makrides, Maria; Collins, Carmel T. (2018-05-31). "A Systematic Review and Meta-Analysis of Human Milk Feeding and Morbidity in Very Low Nativity Weight Infants". Nutrients. 10 (6): 707. doi:10.3390/nu10060707. ISSN 2072-6643. PMC6024377. PMID 29857555.
- ^ a b Quigley, Maria; Embleton, Nicholas D.; McGuire, William (July nineteen, 2019). "Formula versus donor breast milk for feeding preterm or low birth weight infants". The Cochrane Database of Systematic Reviews. seven: CD002971. doi:10.1002/14651858.CD002971.pub5. ISSN 1469-493X. PMC6640412. PMID 31322731.
- ^ Fenton, Tanis R.; Premji, Shahirose Southward.; Al-Wassia, Heidi; Sauve, Reg S. (2014-04-21). "Higher versus lower protein intake in formula-fed depression birth weight infants". The Cochrane Database of Systematic Reviews (four): CD003959. doi:10.1002/14651858.CD003959.pub3. ISSN 1469-493X. PMC7104240. PMID 24752987.
- ^ Ohlsson, Arne; Aher, Sanjay M. (2020-02-11). "Early on erythropoiesis-stimulating agents in preterm or depression birth weight infants". The Cochrane Database of Systematic Reviews. two: CD004863. doi:10.1002/14651858.CD004863.pub6. ISSN 1469-493X. PMC7014351. PMID 32048730.
- ^ Stevens-Simon C, Orleans Chiliad (Sep 1999). "Low-birthweight prevention programs: the enigma of failure". Birth. 26 (3): 184–91. doi:10.1046/j.1523-536x.1999.00184.x. PMID 10655819.
- ^ Kalikkot Thekkeveedu, Renjithkumar; Guaman, Milenka Cuevas; Shivanna, Binoy (November 2017). "Bronchopulmonary dysplasia: A review of pathogenesis and pathophysiology". Respiratory Medicine. 132: 170–177. doi:10.1016/j.rmed.2017.ten.014. ISSN 1532-3064. PMC5729938. PMID 29229093.
- ^ Andrews, K.M.; Brouillette, D.B; Brouillette, R.T. (2008). "Bloodshed, Infant". Encyclopedia of Infant and Early Babyhood Development. pp. 343–359. doi:10.1016/B978-012370877-9.00084-0. ISBN9780123708779.
- ^ Linsell, Louise; Malouf, Reem; Morris, Joan; Kurinczuk, Jennifer J.; Marlow, Neil (Dec 2015). "Prognostic Factors for Poor Cognitive Development in Children Born Very Preterm or With Very Depression Nascency Weight: A Systematic Review". JAMA Pediatrics. 169 (12): 1162–1172. doi:x.1001/jamapediatrics.2015.2175. ISSN 2168-6211. PMC5122448. PMID 26457641.
- ^ Toemen 50., De Jonge Fifty.Fifty., Gishti O., et al Longitudinal growth during fetal life and infancy and cardiovascular outcomes at school-age. J. Hypertens.. 2016;34(7):1396-1406. doi:10.1097/HJH.0000000000000947
- ^ Barker DJ, Osmond C, Forsen TJ, Kajantie E, Eriksson JG. Trajectoriesof growth amid children who have coronary events as adults.North Engl JMed2005; 353:1802–1809.
- ^ Curhan GC, Willett WC, Rimm EB, Spiegelman D, Ascherio AL, Stamp-fer MJ. Birth weight and adult hypertension, diabetes mellitus, andobesity in U.s.a. men.Circulation1996; 94:3246–3250
- ^ Osmond C, Barker DJ, Winter PD, Fall CH, Simmonds SJ. Early growthand death from cardiovascular illness in women.BMJ1993; 307:1519–1524.
- ^ a b c "Global diet targets 2025: depression birth weight policy brief". www.who.int . Retrieved 2020-eleven-04 .
- ^ "UNSD — Methodology: Standard country or area codes for statistical employ (M49)". unstats.un.org . Retrieved 2020-11-04 .
- ^ "FastStats - Birthweight and Gestation". www.cdc.gov. 2020-08-04. Retrieved 2020-11-04 .
- ^ a b Kowlessar Northward.M., Jiang H.J., and Steiner C. Hospital Stays for Newborns, 2011. HCUP Statistical Brief #163. October 2013. Agency for Healthcare Inquiry and Quality, Rockville, Doc. [1]
Source: https://en.wikipedia.org/wiki/Low_birth_weight_babies
0 Response to "Determinants of Low Birth Weight Sex of Babies"
Post a Comment